Improved Treatment of Wet Macular Degeneration
Blog vol 2. 48 Improved treatment of Wet Macular Degeneration
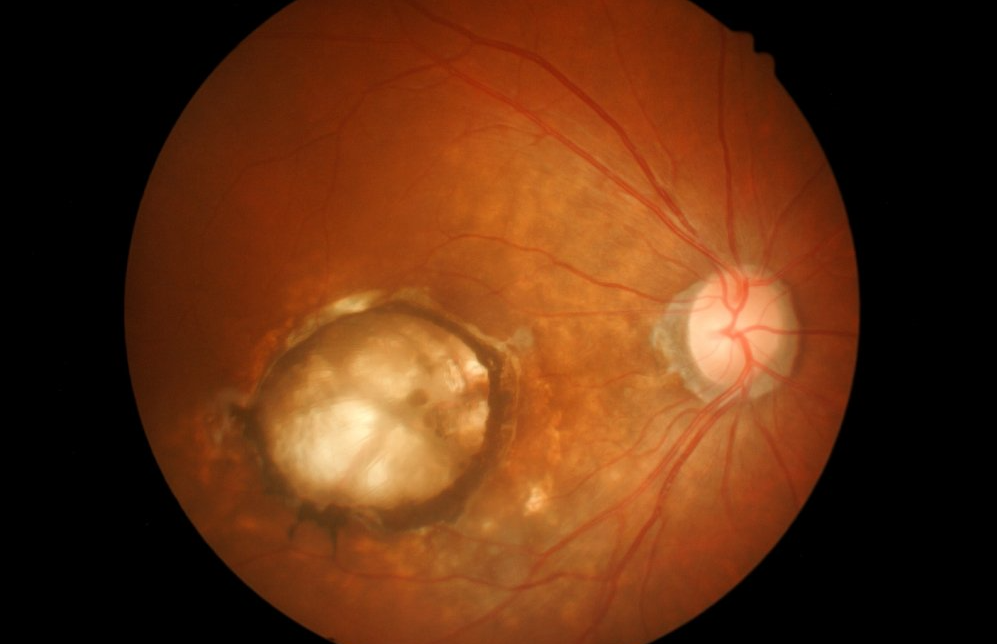
The macula is the center of your vision at the back of the eye. Macular degeneration is a largely hereditary condition associated with aging. There are two kinds: dry and wet.
Wet macular degeneration is when the choroidal vessels near the macula start to leak and the eye starts to form new vessels to compensate, the result, if untreated, is very leaky new vessels and permanent scarring. This used to mean devastating vision loss.
Before the 1990’s this condition was treated with laser and with some improvements, with visudyne and lasers. Then along came a class of drug that works against this new vessel growth and subsequent scarring.
Today, this is the gold standard for treating wet macular degeneration. Drugs like Lucentis or a more recent development, Eylea, are injected into the vitreous of the eye. The first few treatments are monthly, and then if results are good, the injection interval gets extended to as much as 3 months. Drawbacks are the risk of infection and the possibility of endophthalmitis (inflammation of the inside of the eye), as well as the general unpleasantness of the treatment.
A reduction in the number of injections necessary would be good.
A company called Genentech has developed a new drug that is extending this treatment interval. It is called faricimab, and goes by the trade name Vabysmo. The secret in its extensions is its dual action. Unlike its predecessors, that only neutralize the vascular endothelial growth factor-A , faricimab has a complimentary action that neutralizes angiopoietin-2 which also helps to produce these new “leaky” vessels. The additive effect of these two functions equates to less injections. (Read more here).
This is promising for patients and for the health system, making it possible to extend the interval between treatments to at least 4 months.
New methods of delivery are being developed for a current treatment drug, Lucentis. It is called Susvimo by Roche, and uses an implant that releases the drug slowly so that treatments can be done every six months. Down the road, the use of Vabysmo with an implant may get us to an annual treatment. It is all very exciting.
til next week,
the good doctor, Dr. Mark Germain, Burlington optometrist